Pulsed field ablation for cardiac arrythmias: innovating for the future
 By Angelo Auricchio, Chief Medical Officer (CMO), Rhythm Management at Boston Scientific EMEA
By Angelo Auricchio, Chief Medical Officer (CMO), Rhythm Management at Boston Scientific EMEA
I have worked in cardiology for over 30 years, in hospitals, clinical societies and most recently at Boston Scientific. In that time, I have seen first-hand the evolution of treating arrhythmias (heart rhythm disorders), utilising innovation in electrophysiology to treat conditions like paroxysmal and persistent atrial fibrillation (AF) and atrial flutter (AFL). But what’s next in the field, to deliver outcomes for patients, physicians and health systems?
The growing impact of atrial fibrillation and atrial flutter
AF affects approximately 1.5-2% of the general population worldwide.1 Over six million Europeans suffer from AF, and its prevalence is estimated to at least double over the next 50 years as the population ages.2 AFL, while less common than AF, still represents a significant clinical challenge, with an estimated prevalence of 0.1–0.2% in the general population and a strong association with AF – many patients experience both conditions during their lifetime. The number of patients affected, the comorbid impact of stroke, and the cost of both inpatient and outpatient therapy all contribute to an increasing burden on global healthcare systems.3
The growing clinical complexity and systemic impact of AF and AFL means that the need for innovative technologies and devices is more important than ever, to simplify treatment and support system efficiencies while offering safe and effective options for patients.
Evolving cardiac ablation therapy
From its first use in 1998, to its status as a routine management strategy when medication is not an option, our understanding of catheter ablation for AF has grown immensely.4 Over the past 27 years, we have used novel array catheters, mapping systems, and a variety of energy sources to facilitate mapping and ablation for cardiac arrythmias, including thermal energies, laser and cryogenic.5
The most recent (and in my opinion, exciting!) innovation in the field is pulsed field ablation (PFA). PFA uses a purpose-shaped catheter to selectively target heart tissue with an electric field, offering durable ‘silencing’ of abnormal heart signals, and a lower risk of collateral damage to nearby heart structures.6 We are seeing a wealth of evidence for the procedure using the FARAPULSE™ Pulsed Field Ablation Platform, across multiple AF types, patient groups and anatomies.
PFA for patients
PFA also has demonstrable safety benefits, in some cases reporting half the number of adverse events of those associated with radiofrequency ablation.10 Regularly, zero cases of pulmonary vein stenosis are reported following PFA.9, 11 Recent large-scale real-world data with the FARAPULSE PFA Platform further reinforce this favourable safety profile: in a cohort of over 42,000 patients, major adverse events remained below 1%, confirming the consistent safety of PFA.12 When it comes to efficacy, PFA provides high rates of relief from AF, AFL and atrial tachycardia, with very low rates of recurrence.9, 10, 13
PFA for clinical advancement
The therapeutic benefits of PFA in managing various arrhythmias are well established. Moreover, our clinical insights into this modality continue to evolve, opening new pathways for innovation and improved patient outcomes. Leading researchers at this year’s European Society of Cardiology (ESC) congress found that PFA treatment with the FARAPULSE PFA Platform demonstrated less cardiac automatic nervous system (ANS) modulation than cryoballoon ablation, while delivering improved arrhythmia-free outcomes for people living with paroxysmal AF – challenging the currently held idea that cardiac ANS predicts procedural success.14
Recent findings from the ADVANTAGE AF study perfectly illustrate these potential benefits for healthcare professionals, systems and patients. Results from the multicentre evaluation of PFA for typical AFL demonstrated high acute success rates and durable lesion delivery, comparable to established thermal techniques, while maintaining a favourable safety profile. These results underscore the potential of innovative approaches to support workflow efficiencies and improve outcomes for patients and physicians alike.
The next generation of PFA
Building on the transformative nature of PFA is an interesting question and requires us to consider how to innovate beyond an ablation technique.
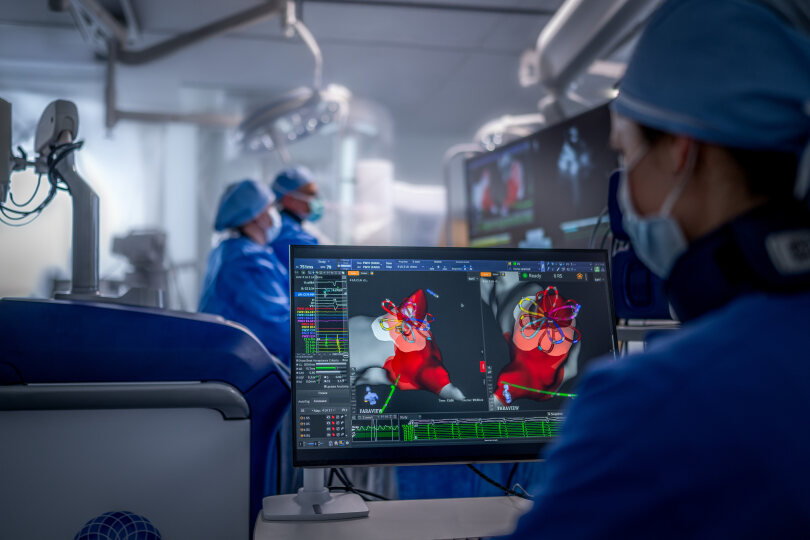
One promising avenue for advancing PFA lies in the evolution of procedural devices, specifically, integrating magnetic navigation capabilities into catheters. This enables both mapping and ablation to be performed using a single device. Traditionally, electrophysiologists relied on separate mapping catheters prior to cardiac PFA procedures to analyse electrical patterns and tailor treatment plans for each patient. Now, paired with advanced software that provides dynamic, 3D visualisation of catheter placement, rotation, and shape in real time, these integrated technologies empower physicians to deliver therapy with greater efficiency and safety. From a health system perspective, the use of a single catheter in PFA procedures introduces new workflow efficiencies. It streamlines care, reduces reliance on fluoroscopy, and may deliver meaningful time and cost savings – benefits that resonate across clinical and operational settings.
Beyond integration, there is significant potential to enhance the power and precision of these devices. Emerging technologies are enabling ablation in more complex regions of the heart, including through scar tissue and within anatomically challenging substrates. PFA is now being explored for ventricular arrhythmias – an area historically considered more difficult to treat due to the proximity of critical structures and the complexity of the underlying tissue. Early clinical experience suggests that PFA may offer a safe, more targeted approach in these cases, with reduced risk of collateral damage and encouraging procedural outcomes.
This expansion into ventricular applications marks a pivotal moment in electrophysiology. It underscores the importance of continued innovation in catheter design, energy delivery, and procedural integration to fully unlock the potential of PFA across a broader spectrum of arrhythmias.
The future of PFA?
As we consider the next chapter in PFA therapy, the possibilities are both exciting and expansive. Whether through continued device innovation, expanded clinical applications, or deeper integration into care pathways, the momentum behind PFA is undeniable. While no one can predict the future with certainty, what we do know is that the clinical evidence supporting new approaches to treating AF continues to grow. At Boston Scientific, we remain committed to driving this innovation forward – collaborating with clinicians, researchers, and health systems to shape the next era of electrophysiology. Here’s to the next 30 years of progress, partnership, and purpose.
The interview was originally published on the Hospital Healthcare Europe website: Pulsed field ablation for cardiac arrythmias: innovating for the future - Hospital Healthcare Europe
CAUTION: The law restricts these devices to sale by or on the order of a physician. Indications, contraindications, warnings and instructions for use can be found in the product labelling supplied with each device or at www.IFU-BSCI.com. Products shown for INFORMATION purposes only and may not be approved or for sale in certain countries. This material is not intended for use in France. 2026 Copyright © Boston Scientific Corporation or its affiliates. All rights reserved. EP-2456504-AA
References:
1 Camm JA et al. 2012 focused update of the ESC Guidelines for the management of atrial fibrillation. European Heart Journal 2012, 33:2719–2747.
2 Guidelines for the management of atrial fibrillation. The task force for the management of atrial fibrillation of the European Society of Cardiology(ESC). Eur. Heart J 2010;31:2369-2449
3 Mayo Clinic. CV Heart Rhythm Services booklet. Available at: http://www.mayoclinic.org/documents/mc5234-23-pdf/doc-20079137. Last accessed September 2025.
4 University of California San Francisco. History of AF Ablation. Available at: https://ucsfhealthcardiology.ucsf.edu/history-af-ablation. Last accessed February 2025.
5 Oral H and Morady F. Ablation of Cardiac Arrhythmias: Past, Present, and Future. AHA Journals. 2024 July; 150(1). doi.org/10.1161/CIRCULATIONAHA.124.068298.
6 Boston Scientific. Atrial Fibrillation Therapy Fact Sheet. Available at: https://www.bostonscientific.com/content/dam/bostonscientific/ep/portfolio-group/single-shot/ablation/desktop/EP-1567605-AA%20BSC%20Atrial%20Fibrillation%20Factsheet.pdf. Last accessed September 2025.
7 Duxbury C, Begley D, Heck PM. Pulsed field ablation with the pentaspline catheter compared with cryoablation for the treatment of paroxysmal atrial fibrillation in the UK NHS: a cost-comparison analysis. BMJ Open 2024;14:e079881. doi:10.1136/bmjopen-2023-079881.
8 Iqbal M et al. Meta-analysis of Pulsed Field Ablation Versus Thermal Ablation for Pulmonary Vein Isolation in AF: A Broad Overview Focusing on Efficacy, Safety and Outcomes. Arrhythmia and Electrophysiology Review 2024;13.
9 Dorset Heart Clinic. Dorset Heart Clinic becomes only private centre in Dorset licensed to perform Pulse Field Ablation procedures for Atrial Fibrillation. Available at: https://dorsetheartclinic.co.uk/farapulse/. Last accessed September 2025.
10 Boersma L et al. Real-world experience with the pentaspline pulsed field ablation system: one-year outcomes of the FARADISE registry. Europace 2025;27;9. doi.org/10.1093/europace/euaf182
11 Reddy V et al. Pulsed Field Ablation of Persistent Atrial Fibrillation With Continuous Electrocardiographic Monitoring Follow-Up: ADVANTAGE AF Phase 2. Circulation 2025;152;1. doi.org/10.1161/CIRCULATIONAHA.125.074485
12 Turagam, M, Aryana, A, Day, J. et al. Multicenter Study on the Safety of Pulsed Field Ablation in Over 40,000 Patients: MANIFEST-US. JACC. null2025, 0 (0). https://doi.org/10.1016/j.jacc.2025.10.051
13 Reichlin T et al. Pulsed Field or Cryoballoon Ablation for Paroxysmal Atrial Fibrillation. N Engl J Med 2025;392:1497-1507. DOI: 10.1056/NEJMoa2502280
14 Roten L et al. SINGLE SHOT CHAMPION Trial - Autonomic effects and ablation success after pulsed field and cryoballoon ablation. Presented at European Society of Cardiology Congress 2025. Available at: https://esc365.escardio.org/presentation/312425